A new insight into the molecular hydrogen effect on coenzyme Q and mitochondrial function of rats
Abstract
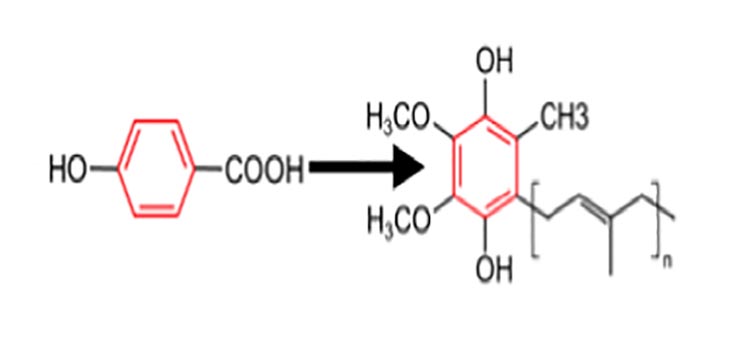
Mitochondria are the major source of cellular energy metabolism. In the cardiac cells, mitochondria produce by way of the oxidative phosphorylation more than 90% of the energy supply in the form of ATP, which is utilized in many ATP-dependent processes, like cycling of the contractile proteins or maintaining ion gradients. Reactive oxygen species (ROS) are by-products of cellular metabolism and their levels are controlled by intracellular antioxidant systems. Imbalance between ROS and the antioxidant defense leads to oxidative stress and oxidative changes to cellular biomolecules. Molecular hydrogen (H2) has been proved as beneficial in the prevention and therapy of various diseases including cardiovascular disorders. It selectively scavenges hydroxyl radical and peroxynitrite, reduces oxidative stress, and has anti-inflammatory and anti-apoptotic effects. The effect of H2 on the myocardial mitochondrial function and coenzyme Q levels is not well known. In this paper, we demonstrated that consumption of H2-rich water (HRW) resulted in stimulated rat cardiac mitochondrial electron respiratory chain function and increased levels of ATP production by Complex I and Complex II substrates. Similarly, coenzyme Q9 levels in the rat plasma, myocardial tissue, and mitochondria were increased and malondialdehyde level in plasma was reduced after HRW administration. Based on obtained data, we hypothesize a new metabolic pathway of the H2 effect in mitochondria on the Q-cycle and in mitochondrial respiratory chain function. The Q-cycle contains three coenzyme Q forms: coenzyme Q in oxidized form (ubiquinone), radical form (semiquinone), or reduced form (ubiquinol). H2 may be a donor of both electron and proton in the Q-cycle and thus we can suppose stimulation of coenzyme Q production. When ubiquinone is reduced to ubiquinol, lipid peroxidation is reduced. Increased CoQ9 concentration can stimulate electron transport from Complex I and Complex II to Complex III and increase ATP production via mitochondrial oxidative phosphorylation. Our results indicate that H2 may function to prevent/treat disease states with disrupted myocardial mitochondrial function.
See the study at National Library of Medicine